Advancements in Pancreatic Cancer Surgery
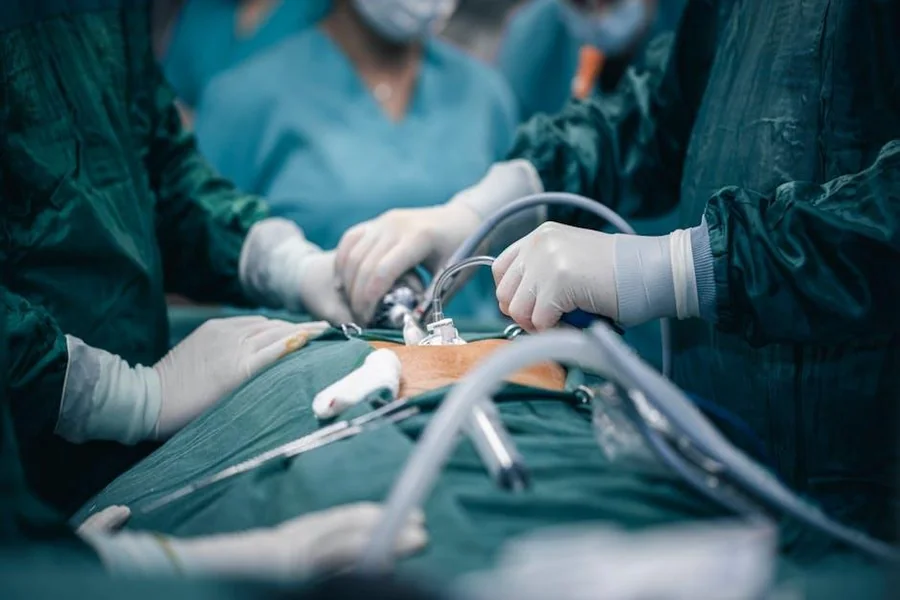
Pancreatic cancer is notorious for its aggressive nature and challenging treatment regimen. Surgical intervention remains the cornerstone for a potential cure, yet only a fraction of patients qualify for surgical procedures due to the late presentation of the disease. For more detailed insights into this condition, you can visit https://www.drthngyongxian.com/pancreatic-cancer/. In recent years, significant advancements in surgical techniques and perioperative care have emerged, providing hope for patients facing this formidable disease. To explore more about the intricacies of pancreatic cancer, visit this comprehensive resource on pancreatic cancer.
Challenges and Considerations in Pancreatic Cancer Surgery
Pancreatic surgery, often termed as pancreaticoduodenectomy or the Whipple procedure, is intricate and demanding. It is mainly indicated for tumours located in the head of the pancreas. Due to the proximity of the pancreas to major blood vessels, the surgical procedure requires meticulous planning and precision. Preoperative assessments, including imaging studies and laparoscopy, are critical for evaluating tumour resectability.
Surgical Techniques and Innovations
In recent years, surgical techniques have evolved, incorporating minimally invasive approaches that offer patients better postoperative recovery and reduced hospital stays. Laparoscopic and robot-assisted surgeries have become increasingly prevalent, allowing for greater precision and control during operations. Surgeons have made strides in reducing operative time and improving patient outcomes through these advanced techniques.
Vascular resections and reconstructions, while complex, are often necessary during pancreatic surgery due to the tumour’s location. Advances in this area now allow surgeons to achieve clear margins while maintaining vascular integrity, which is crucial for disease-free survival.
Perioperative and Postoperative Management
The success of pancreatic surgery depends significantly on meticulous perioperative management. Enhanced recovery after surgery (ERAS) protocols have been developed to optimise patient outcomes. These protocols encompass pain management, nutritional support, and early mobilisation, each of which significantly influence recovery trajectories.
Early Detection and Screening Strategies for Pancreatic Cancer
Early detection of pancreatic cancer is crucial, as surgical eligibility is often limited to patients diagnosed at an operable stage. This topic can cover current screening methods, including imaging techniques like CT scans, MRI, and endoscopic ultrasound, as well as emerging biomarkers and genetic testing for high-risk individuals. Emphasising early detection helps improve patient outcomes and increases the likelihood of successful surgical intervention.
Minimally Invasive Surgery vs. Open Surgery: Pros and Cons
An in-depth discussion comparing minimally invasive techniques (laparoscopic and robot-assisted surgeries) with traditional open surgeries. Highlight recovery time, complication rates, precision, and patient suitability for each method. Th
Pain Management and Nutritional Support Post-Surgery
Postoperative care is a critical component of recovery. This topic can focus on pain control strategies, including multimodal analgesia, and nutritional interventions such as enteral feeding or pancreatic enzyme supplementation. Proper management enhances recovery speed, reduces complications, and improves overall quality of life.
Advances in Multidisciplinary Care and Oncology Collaboration
Pancreatic cancer treatment is most effective when multiple specialities collaborate. This topic explores how surgical teams work alongside oncologists, radiologists, and palliative care specialists, highlighting the role of integrated treatment plans, neoadjuvant and adjuvant therapies, and clinical trial participation.
Postoperative complications are not uncommon, with pancreatic fistula being among the most dreaded. However, current management strategies, including prophylactic measures and early intervention protocols, have reduced the incidence and severity of such complications.
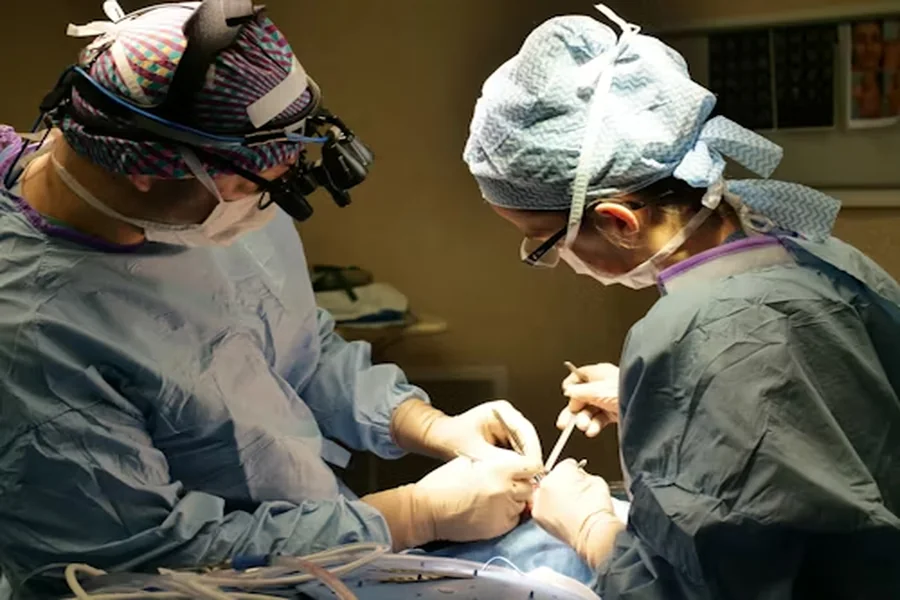
Multidisciplinary Approaches in Treatment
Pancreatic cancer treatment extends beyond surgical intervention, necessitating a comprehensive, multidisciplinary approach. The integration of oncologists, radiologists, pathologists, and supportive care teams ensures that each patient receives a tailored treatment plan. Neoadjuvant and adjuvant therapies continue to play a pivotal role in managing pancreatic cancer, improving surgical outcomes and overall survival rates.
Participation in clinical trials provides patients with access to innovative therapies and protocols, fostering advancements in pantherapy. Continual research and collaboration among healthcare professionals drive the evolution of treatment modalities.
Future Innovations in Pancreatic Cancer Treatment
Looking ahead, this topic covers emerging research in personalised medicine, immunotherapy, targeted molecular therapies, and AI-assisted surgical planning. Discussing these innovations offers hope for improved survival rates and better patient outcomes in the coming years.
Outlook and Future Directions
The landscape of pancreatic cancer surgery is continually evolving, with ongoing research focused on improving surgical techniques and patient outcomes. Molecular profiling and personalised medicine are emerging as focal areas, offering new opportunities for targeted therapies that complement surgical intervention.
Overall, these advancements underscore a commitment to improving the quality of life and survival rates for patients with pancreatic cancer. By staying informed about the latest developments and engaging with healthcare professionals, patients can access a wider array of treatment options and make informed decisions about their care.
Conclusion: Progress and Hope in Pancreatic Cancer Care
Advancements in pancreatic cancer surgery reflect a broader commitment to improving patient outcomes despite the disease’s complexity and aggressiveness. From minimally invasive surgical techniques to multidisciplinary care and personalised treatment plans, modern approaches are continually enhancing survival rates and quality of life. While challenges remain, ongoing research, early detection strategies, and emerging therapies provide hope for patients and their families. Staying informed and engaging with experienced healthcare professionals empowers patients to make well-considered decisions, ensuring that each step of their treatment journey is guided by the latest innovations and best practices.
